You get your blood work back. There’s a page full of numbers, abbreviations, and little H and L flags next to some of them. Your doctor says everything looks “basically fine” but doesn’t have time to explain what you’re looking at. You go home and Google “low MCH” and end up down a rabbit hole that convinces you something is seriously wrong.
This happens constantly. And it happens because most CBC explanations are either too vague to be useful or too technical to be readable.
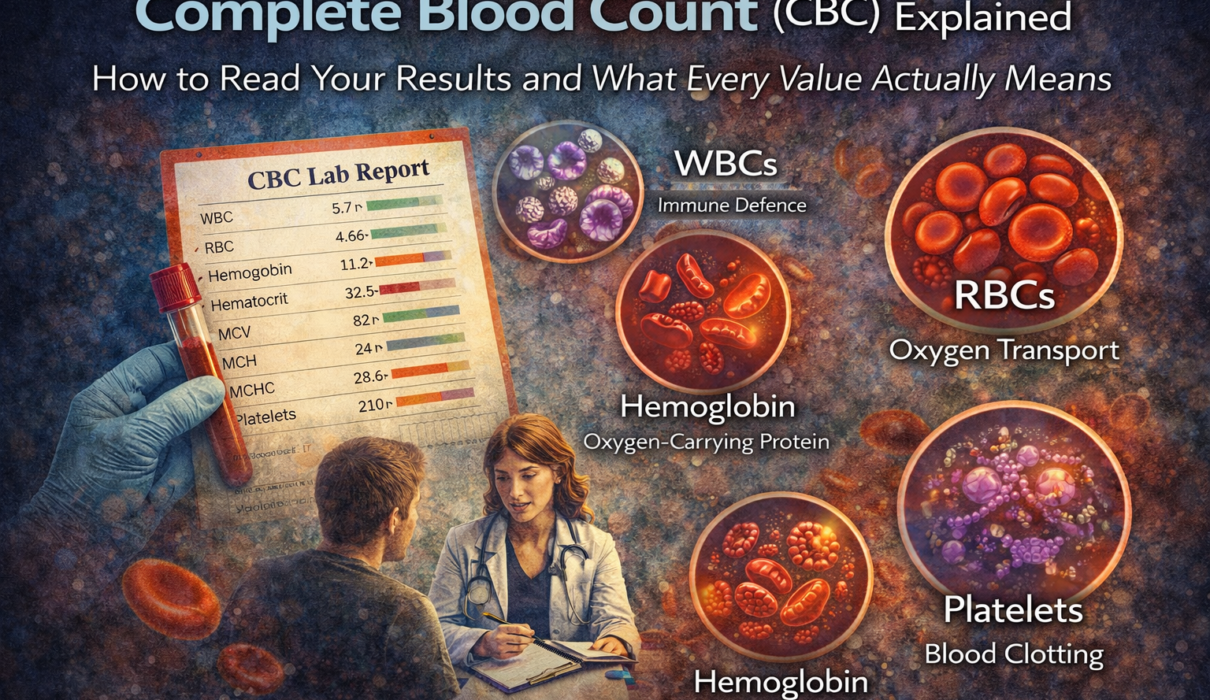
The CBC – complete blood count – is the most commonly ordered blood test in American medicine. Your doctor has likely ordered one at almost every physical you’ve ever had. It gives a snapshot of your blood’s three main cell types and what they’re doing. Understanding what it actually measures, what the numbers mean, and when an abnormal flag is genuinely worth worrying about versus when it’s noise – that’s what this article is for.
One important note upfront: lab reference ranges vary slightly between laboratories depending on their equipment and the population they calibrate against. The ranges given here reflect standard adult reference values used across most US clinical laboratories, but always read your result against the reference range printed on your own lab report.
What a CBC actually measures
Blood is made up of three main cell types, each produced in the bone marrow and each doing a specific job. The CBC counts and characterizes all three, plus gives you several calculated indices that help interpret what those counts mean.
The three main components are red blood cells (which carry oxygen), white blood cells (which drive immune response), and platelets (which control bleeding). A standard CBC report will give you somewhere between 15 and 20 individual values covering all three, plus a differential breakdown of the different white blood cell subtypes.
Let’s go through each section properly.
Red blood cell (RBC) section
This is usually the most clinically significant part of the CBC for most patients, because abnormalities here – particularly anemia – are extremely common and have practical implications for how you feel day to day.
RBC count
This is simply the number of red blood cells per microliter of blood.
| Men | Women | |
|---|---|---|
| Normal range | 4.5 – 5.9 million/µL | 4.0 – 5.2 million/µL |
Women have a naturally lower RBC count than men – primarily because menstruation causes regular blood loss, and estrogen slightly suppresses red cell production compared to testosterone. This is normal physiology, not a problem.
A low RBC count points toward anemia, which has many possible causes. A high count (called polycythemia) can occur in people who live at altitude, in smokers, in people with certain lung conditions that cause chronically low oxygen, or – rarely – due to bone marrow disorders.
Hemoglobin (Hgb or Hb)
Hemoglobin is the protein inside red blood cells that actually binds and carries oxygen. It’s the most clinically important single value in the red cell section – more so than the raw RBC count – because it directly reflects the blood’s oxygen-carrying capacity.
| Men | Women | |
|---|---|---|
| Normal range | 13.5 – 17.5 g/dL | 12.0 – 15.5 g/dL |
Hemoglobin below the lower limit of normal in the context of symptoms (fatigue, breathlessness, pallor, cold intolerance) is the standard diagnostic threshold for anemia. Below around 10 g/dL, most people feel meaningfully symptomatic. Below 7-8 g/dL, transfusion is often considered.
Hematocrit (Hct)
Hematocrit is the percentage of total blood volume made up of red blood cells. It tracks closely with hemoglobin and conveys similar information – roughly, hematocrit is about three times the hemoglobin value in a healthy person.
| Men | Women | |
|---|---|---|
| Normal range | 41 – 53% | 36 – 46% |
Dehydration is one of the most common causes of a mildly elevated hematocrit – when plasma volume drops, the red cell percentage appears higher without any actual increase in red cell production.
The red cell indices – MCV, MCH, MCHC, RDW
These calculated values describe the characteristics of individual red blood cells rather than just how many there are. They’re especially useful for figuring out what type of anemia someone has, which matters because different types need different treatments.
MCV (Mean Corpuscular Volume) – the average size of red blood cells, measured in femtoliters (fL).
Normal range: 80 – 100 fL
- Low MCV (microcytic anemia, cells too small): most commonly iron deficiency anemia. Also thalassemia, chronic disease.
- Normal MCV (normocytic anemia): chronic disease, kidney disease, mixed deficiencies, early iron deficiency, bone marrow problems.
- High MCV (macrocytic anemia, cells too large): vitamin B12 deficiency, folate deficiency, alcohol use, hypothyroidism, certain medications (especially methotrexate, hydroxyurea).
MCH (Mean Corpuscular Hemoglobin) – the average amount of hemoglobin per red blood cell, in picograms (pg).
Normal range: 27 – 33 pg
MCH moves in the same direction as MCV in most cases. Low MCH (hypochromic cells, pale-looking) typically accompanies iron deficiency. High MCH accompanies B12 or folate deficiency.
MCHC (Mean Corpuscular Hemoglobin Concentration) – hemoglobin concentration within the average red blood cell.
Normal range: 31 – 37 g/dL
This is less clinically dramatic than MCV and MCH in most cases. A notably low MCHC confirms hypochromia (pale, iron-deficient cells). A high MCHC can occasionally flag hereditary spherocytosis.
RDW (Red Cell Distribution Width) – a measure of how much variation there is in red blood cell size. Think of it as a consistency score.
Normal range: 11.5 – 14.5%
A high RDW means your red cells are varying significantly in size – some very small, some very large. This pattern shows up in mixed deficiency anemias (iron plus B12, for example), early iron deficiency before the MCV has dropped, and certain hemolytic anemias. A normal RDW alongside a low MCV strongly suggests thalassemia trait rather than iron deficiency.
“The red cell indices – particularly MCV and RDW together – are how hematologists distinguish between different types of anemia without additional tests. Iron deficiency classically gives low MCV with high RDW. Thalassemia trait gives low MCV with normal RDW. B12 deficiency gives high MCV, often with high RDW. These patterns are one of the most elegant examples of how a simple blood count can do a lot of diagnostic work.”
White blood cell (WBC) section
White blood cells are your immune system’s active cell force. The total WBC count tells you whether there are more or fewer immune cells than expected. The differential tells you which type is driving that change – and that’s where the clinically useful information lives.
Total WBC count
Normal range: 4,500 – 11,000 cells/µL (or 4.5 – 11.0 × 10³/µL)
A high WBC count (leukocytosis) most commonly reflects an active infection, usually bacterial. It also occurs with significant physical or emotional stress, steroid use, and in smokers (who have chronically elevated WBCs). A dramatically elevated count can indicate leukemia, though this is far less common than infection.
A low WBC count (leukopenia) can occur with viral infections (particularly the flu or COVID-19), certain autoimmune conditions, bone marrow suppression from chemotherapy or radiation, and some medications.
The differential – five white cell types
A standard CBC with differential breaks the total WBC count into five types. Each type has a specific immune function, and knowing which type is elevated or low tells you something about what the body is responding to.
| Cell type | Normal % of total WBC | Normal absolute count | Primary role |
|---|---|---|---|
| Neutrophils | 50 – 70% | 1,800 – 7,700/µL | First responders to bacterial infection and tissue injury |
| Lymphocytes | 20 – 40% | 1,000 – 4,800/µL | Viral immunity, antibody production (B cells), cellular immunity (T cells) |
| Monocytes | 2 – 8% | 200 – 950/µL | Chronic infection, inflammation, tissue cleanup |
| Eosinophils | 1 – 4% | 15 – 500/µL | Allergic responses, parasitic infection |
| Basophils | 0.5 – 1% | 0 – 100/µL | Allergic and inflammatory reactions |
Neutrophilia (high neutrophils) – the most common WBC abnormality. Bacterial infection is the classic cause. Also seen with stress, corticosteroid use, and significant physical exertion.
Lymphocytosis (high lymphocytes) – typical of viral infections. A dramatically elevated lymphocyte count with atypical-looking cells on the blood smear is the classic pattern of infectious mononucleosis (mono).
Eosinophilia (high eosinophils) – the two most common causes in the US are allergic conditions (asthma, eczema, hay fever) and parasitic infections. A persistently elevated eosinophil count is worth investigating.
Neutropenia (low neutrophils) – clinically significant when severe (below 1,000/µL) because it significantly impairs the ability to fight bacterial infections. Can be caused by viral infections, autoimmune conditions, certain medications, or bone marrow problems. Chemotherapy-related neutropenia is common and carefully monitored.
Platelet section
Platelet count
Platelets are the tiny cell fragments responsible for forming clots when you bleed. They aggregate at the site of vessel injury and form the initial plug that stops bleeding.
Normal range: 150,000 – 400,000/µL (or 150 – 400 × 10³/µL)
Low platelets (thrombocytopenia) – below 150,000/µL. Spontaneous bleeding risk becomes significant when counts fall below 50,000/µL, and severe risk below 20,000/µL. Causes include immune thrombocytopenic purpura (ITP), viral infections, certain medications, liver disease, and – in hospitalized patients – heparin-induced thrombocytopenia.
High platelets (thrombocytosis) – above 400,000/µL. Reactive thrombocytosis following surgery, infection, or iron deficiency is common and usually resolves on its own. Persistent marked elevation (above 1,000,000/µL) may indicate a myeloproliferative disorder and requires investigation.
MPV (Mean Platelet Volume)
Normal range: 7.5 – 12.5 fL
MPV measures the average size of platelets. Larger platelets are generally younger and more metabolically active. A low platelet count with high MPV suggests the bone marrow is trying to compensate by releasing larger, younger platelets – as in ITP. Low platelet count with low MPV suggests reduced production – as in aplastic anemia or bone marrow suppression.
How to read your own CBC report
When your results come back, here’s a practical approach to reading them without panicking or dismissing things you shouldn’t:
Step 1: Look at which values are flagged. Most lab reports mark values outside the reference range with H (high) or L (low). Start there rather than trying to interpret every number.
Step 2: Check the magnitude of the abnormality. A hemoglobin of 12.8 g/dL in a woman (just below the 13.5 cutoff some labs use) is very different from a hemoglobin of 8.5 g/dL. Context and degree matter enormously.
Step 3: Look for patterns, not isolated values. A single low value often means less than a pattern across related values. Low hemoglobin + low MCV + low MCH + high RDW together point clearly toward iron deficiency. That constellation is more significant than any single number flagged.
Step 4: Connect results to symptoms. An isolated mildly low WBC in a healthy person who feels completely fine is usually not the same clinical situation as a low WBC in someone who has been running fevers and feeling exhausted. Lab values and clinical picture always go together.
Step 5: Ask your doctor specifically what the abnormal values mean for you. You’re entitled to that explanation. “My hemoglobin is flagged low – what does that mean and do I need to do anything about it?” is a completely reasonable question to bring to any appointment.
“A single abnormal value on a CBC is often not the beginning of a serious diagnosis. It’s a question mark that needs context – your symptoms, your history, your other values, and sometimes a repeat test. The CBC is a screening tool, not a verdict.”
Common CBC patterns and what they suggest
| Pattern | What it suggests | Common causes |
|---|---|---|
| Low Hgb + Low MCV + Low MCH + High RDW | Microcytic hypochromic anemia | Iron deficiency (most common), chronic blood loss |
| Low Hgb + Low MCV + Normal RDW | Microcytic anemia with uniform cells | Thalassemia trait |
| Low Hgb + High MCV + High RDW | Macrocytic anemia | B12 deficiency, folate deficiency, alcohol use |
| Low Hgb + Normal MCV + Normal RDW | Normocytic anemia | Chronic disease, kidney disease, early iron deficiency |
| High WBC + High neutrophils | Leukocytosis with neutrophilia | Bacterial infection, stress response, steroid use |
| High WBC + High lymphocytes | Leukocytosis with lymphocytosis | Viral infection (including mono, COVID-19) |
| High eosinophils | Eosinophilia | Allergic condition, parasitic infection |
| Low platelets | Thrombocytopenia | ITP, viral infection, medications, liver disease |
| High MCV + Normal Hgb | Macrocytosis without anemia | B12/folate deficiency (early), alcohol, hypothyroidism |
FAQs
My CBC came back with a flagged value but my doctor said it’s fine. Should I be worried? Not necessarily. Doctors routinely see flagged values that fall just outside reference ranges, are stable compared to previous results, and have no clinical significance given your symptoms and history. Reference ranges are statistical constructs – they’re set so that 95% of healthy people fall within them, which means 5% of healthy people will have at least one value outside the range by chance alone. A single mildly abnormal value without symptoms or a clinical story to match it is often monitored rather than acted on.
What’s the difference between a CBC and a CBC with differential? A basic CBC gives you the total counts for red cells, white cells, and platelets, plus the red cell indices. A CBC with differential additionally breaks down the white blood cell count into its five component types (neutrophils, lymphocytes, monocytes, eosinophils, basophils). Most doctors order the differential routinely – it provides significantly more clinical information and is what this article has covered throughout.
Can dehydration affect my CBC results? Yes – significantly. Dehydration reduces plasma volume (the liquid portion of blood), which concentrates the cellular components. This can cause artificially elevated hemoglobin, hematocrit, and red blood cell counts. It’s one reason labs ask whether you’ve been drinking normally before a blood draw. If your CBC shows high-normal or elevated hematocrit without other findings, mild dehydration is often the explanation.
Should I fast before a CBC? Fasting isn’t typically required for a CBC alone – unlike cholesterol or blood sugar tests. However, if your CBC is being drawn as part of a comprehensive metabolic panel or lipid profile, fasting for 9-12 hours before may be required for those other tests. Check with your ordering provider if you’re unsure.
How often should a CBC be done? For healthy adults with no known conditions, a CBC is typically included in routine annual bloodwork or during periodic health checkups. People with chronic conditions like anemia, immune disorders, kidney disease, or those on medications that affect blood counts may need more frequent monitoring – your doctor will advise based on your specific situation.
Disclaimer
This article is for educational purposes only and does not constitute medical advice. CBC reference ranges vary between laboratories – always interpret your results against the specific reference range printed on your own lab report. Abnormal values should be discussed with your healthcare provider, who can interpret them in the context of your symptoms, medical history, and other test results. Do not use this article to self-diagnose or change your treatment without consulting a qualified healthcare professional.
References
- Bain BJ, Bates I, Laffan MA. (2017). Dacie and Lewis Practical Haematology (12th ed.). Elsevier.
- MedlinePlus. (2024). Complete blood count (CBC). National Library of Medicine. https://medlineplus.gov/lab-tests/complete-blood-count-cbc/
- Mayo Clinic Laboratories. (2024). CBC with differential reference ranges. https://www.mayocliniclabs.com
- Tefferi A, Hanson CA, Inwards DJ. (2005). How to interpret and pursue an abnormal complete blood cell count in adults. Mayo Clinic Proceedings, 80(7), 923-936. https://doi.org/10.4065/80.7.923
- National Heart, Lung, and Blood Institute. (2024). Blood tests. https://www.nhlbi.nih.gov/health-topics/blood-tests
- Buttarello M, Plebani M. (2008). Automated blood cell counting: state of the art. American Journal of Clinical Pathology, 130(1), 104-116. https://doi.org/10.1309/EK3C7CTDKNVPXVTN
- Lippi G, Plebani M. (2014). Integrated diagnostics: the future of laboratory medicine. Biochemia Medica, 24(2), 220-225. https://doi.org/10.11613/BM.2014.024
- American Society of Hematology. (2024). Blood basics. https://www.hematology.org/education/patients/blood-basics




3 Comments