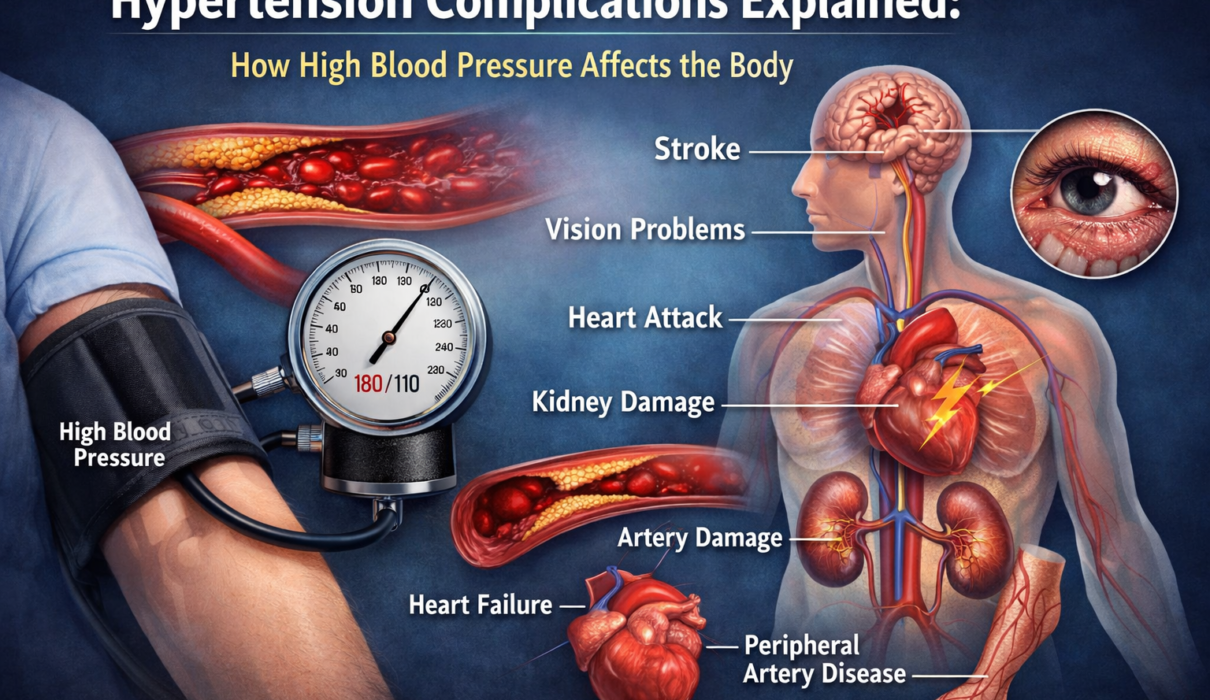
Hypertension is called the silent killer not because it’s rare or unpredictable – it’s the most common chronic condition in American adults – but because the damage it causes accumulates invisibly over years. By the time symptoms appear, something has already gone significantly wrong. A heart attack. A stroke. Kidney failure quietly discovered on routine bloodwork. Vision loss that emerged without warning.
This article explains organ by organ what persistently elevated blood pressure actually does to the body, the mechanisms behind each complication, and which ones represent the most serious long-term risks.
Why Complications Develop: The Shared Mechanism
Before going organ by organ, it’s worth understanding the two core mechanisms that almost all hypertension complications share.
Endothelial injury and atherosclerosis: The inner lining of blood vessels – the endothelium – is a single layer of cells that plays an active role in regulating vascular tone, preventing clot formation, and controlling inflammation. Sustained elevated pressure physically damages these cells, triggering an inflammatory response. Damaged endothelium becomes more permeable to LDL cholesterol particles, which deposit in the arterial wall and set off the atherosclerotic process – plaque formation, arterial narrowing, reduced blood flow. This process affects every arterial bed in the body.
Pressure overload on organs: Some organs – particularly the heart, kidneys, and brain – receive blood under direct arterial pressure. Sustained high pressure acts as a mechanical stress on these tissues, causing structural changes over time: the heart wall thickens, glomeruli in the kidneys scar, and small arteries in the brain become thickened and prone to rupture or occlusion.
Both processes are silent, cumulative, and largely irreversible once established – which is why the goal of treatment is prevention, not repair.
The Heart: The Organ Under the Greatest Strain
The heart bears the most direct burden of hypertension. Every beat, it pumps against higher-than-normal arterial pressure – the equivalent of pumping water through a narrower pipe. Over years, this creates several distinct cardiac complications:
Left Ventricular Hypertrophy (LVH)
The left ventricle – the main pumping chamber – responds to chronic pressure overload by thickening its walls. This initially maintains pumping ability, but the thickened muscle becomes stiffer and less compliant, making it harder for the chamber to relax and fill between beats. LVH is detectable on echocardiogram before symptoms appear and is an independent predictor of heart attack, heart failure, sudden cardiac death, and stroke.
Heart Failure
Hypertension is the single most common risk factor for heart failure in the US, accounting for approximately 75% of cases according to AHA data. Two patterns emerge: heart failure with preserved ejection fraction (where the ventricle stiffens and can’t fill properly despite normal squeeze function – the dominant pattern in hypertension-related failure) and heart failure with reduced ejection fraction (where the muscle eventually weakens and dilates after years of overwork). Both cause shortness of breath, fatigue, and reduced exercise capacity.
Coronary Artery Disease
Hypertension accelerates atherosclerosis in the coronary arteries through endothelial injury and oxidative stress. Narrowed coronary arteries reduce blood flow to the heart muscle, causing angina (chest pain on exertion) and eventually heart attack if a plaque ruptures and a clot blocks the vessel. People with hypertension have approximately twice the risk of coronary artery disease compared to those with normal blood pressure.
Atrial Fibrillation
Structural changes from hypertension – particularly elevated filling pressure in the left ventricle that backs up into the left atrium – cause the left atrium to dilate and develop fibrotic changes. This creates the electrical disorganization that drives atrial fibrillation (AFib), the most common sustained cardiac arrhythmia. Hypertension is the single most common modifiable risk factor for AFib. The consequence is significant: AFib increases stroke risk fivefold, and the strokes it causes tend to be larger and more disabling than other stroke types.
The Brain: Stroke, Hemorrhage, and Cognitive Decline
The brain is exquisitely sensitive to changes in blood pressure and blood flow. Hypertension affects the brain through several distinct pathways.
Stroke
Hypertension is the single most important modifiable risk factor for stroke – responsible for approximately 54% of strokes globally, according to a major meta-analysis in The Lancet. It contributes to both major stroke types:
Ischemic stroke (80-85% of strokes): Hypertension accelerates atherosclerosis in the large and medium arteries supplying the brain, and promotes small vessel disease (lacunar strokes) in the deep brain. Blood pressure-related AFib also drives cardioembolic stroke.
Hemorrhagic stroke (15-20% of strokes): When chronically elevated pressure weakens and eventually ruptures small penetrating arteries deep in the brain, a hemorrhagic stroke results. These are often devastating and heavily associated with severely uncontrolled hypertension.
Reducing blood pressure by 10 mmHg systolic lowers stroke risk by approximately 35%, according to meta-analyses of blood pressure-lowering trials.
Transient Ischemic Attack (TIA)
A TIA – sometimes called a “mini-stroke” – produces temporary neurological symptoms (facial drooping, arm weakness, speech difficulty, vision changes) that resolve within 24 hours. TIAs are driven by the same mechanisms as ischemic stroke and are a strong warning sign: the 90-day stroke risk after a TIA is approximately 10-15%, with the highest risk in the first 48 hours. Any TIA requires urgent medical evaluation.
Hypertensive Encephalopathy
In hypertensive emergency – when blood pressure rises very rapidly to extreme levels – the brain’s autoregulation (its ability to maintain stable blood flow despite varying systemic pressure) can be overwhelmed. Blood vessels dilate passively, and fluid leaks into brain tissue producing cerebral edema. Symptoms include severe headache, confusion, visual disturbances, seizures, and altered consciousness. This is a medical emergency requiring immediate treatment.
Cognitive Decline and Dementia
Midlife hypertension is increasingly recognized as a major risk factor for cognitive impairment and dementia decades later. The mechanisms include accumulation of small vessel disease (white matter changes visible on MRI), subclinical lacunar infarcts, reduced cerebral blood flow, and possibly direct neurodegenerative effects. Data from the SPRINT-MIND trial found that intensive blood pressure lowering (targeting below 120 mmHg systolic) significantly reduced the risk of mild cognitive impairment – the precursor state to dementia – compared to standard treatment.
The Kidneys: A Silent Deterioration
Hypertension damages the kidneys gradually through glomerulosclerosis (scarring of the kidney’s filtering units), arteriosclerosis of the renal arterioles, and tubular injury from reduced blood flow. This process – hypertensive nephrosclerosis – typically produces no symptoms until substantial function has been lost.
Hypertension is the second leading cause of kidney failure in the US after diabetes. The kidney damage is detectable early through urine albumin testing (proteinuria appears before eGFR falls) and through tracking eGFR over time.
What makes the kidney-hypertension relationship particularly insidious is that it’s bidirectional: damaged kidneys raise blood pressure further through fluid retention and RAAS overactivation, creating a cycle that accelerates both conditions simultaneously. This is covered in depth in the dedicated Hypertension and Kidney Health article on this site.
The Eyes: Hypertensive Retinopathy
The retina – the light-sensitive tissue at the back of the eye – contains a dense network of small blood vessels that are highly visible on fundoscopic examination. These vessels are directly affected by sustained elevated pressure, producing a spectrum of changes called hypertensive retinopathy.
Early changes include arteriolar narrowing (the vessels constrict in response to pressure) and arteriovenous nicking (where thickened arteries compress the veins that cross them). More advanced changes include flame-shaped hemorrhages, cotton-wool spots (areas of retinal ischemia), and in severe hypertension, papilledema (swelling of the optic disc).
Most people with hypertensive retinopathy have no visual symptoms until changes are advanced. This is another reason why routine blood pressure control protects health that isn’t “felt” – optic changes are often discovered by an ophthalmologist during a routine eye exam in someone who had no idea their blood pressure was affecting their vision.
Severe hypertensive retinopathy in the context of hypertensive emergency can cause rapid visual deterioration and requires urgent blood pressure reduction.
The Blood Vessels: Peripheral Disease and Aneurysm
Peripheral Artery Disease (PAD)
Hypertension accelerates atherosclerosis in the arteries of the lower limbs, reducing blood flow. Early PAD produces cramping leg pain during walking (claudication) that resolves with rest. Advanced PAD can cause rest pain, non-healing wounds, and in severe cases limb-threatening ischemia. People with hypertension have approximately double the risk of PAD.
Aortic Aneurysm
The aorta bears the highest pressure in the body with every heartbeat. Sustained hypertension weakens the aortic wall over time, leading to progressive dilation. An aortic aneurysm – a bulge in the aortic wall – is typically asymptomatic until it ruptures, at which point mortality is very high. Aortic aneurysm risk is significantly elevated in people with long-standing hypertension, particularly smokers.
Aortic Dissection
In hypertensive emergency or in individuals with connective tissue disorders, the extreme forces on the aortic wall can cause the inner layers to tear apart – a dissection. This is one of the most dramatic cardiovascular emergencies, typically presenting with sudden, severe chest or back pain described as “tearing” or “ripping.” It requires immediate emergency treatment.
Sexual Health Complications
Erectile dysfunction is significantly more prevalent in men with hypertension, occurring in roughly 30-50% of men with the condition. The mechanism is vascular – hypertension impairs endothelial function and reduces arterial blood flow to erectile tissue. This is often compounded by some antihypertensive medications (particularly older beta-blockers and diuretics at higher doses). ACE inhibitors, ARBs, and calcium channel blockers tend to have neutral or less negative effects on sexual function and are often preferred for this reason.
What Determines Whether Complications Develop
Not everyone with hypertension develops all – or any – of these complications. The key determinants are:
- Duration of hypertension – longer exposure means more cumulative damage
- Severity of elevation – higher pressures cause faster and more severe damage
- Blood pressure variability – fluctuating pressure (even averaging the same) may cause more damage than stable pressure at the same mean level
- Coexisting risk factors – diabetes, smoking, high LDL, obesity, and CKD all multiply cardiovascular risk
- Treatment – effective blood pressure control substantially reduces the risk of all these complications
The risk reduction from treatment is real and well-documented. A 10 mmHg reduction in systolic blood pressure reduces major cardiovascular events by approximately 20-25%, stroke by 35%, and heart failure by 40%, based on meta-analyses of blood pressure-lowering trials.
Frequently Asked Questions
At what blood pressure level do complications start occurring? The relationship between blood pressure and cardiovascular risk is continuous – there’s no sharp threshold below which risk is zero. Risk starts rising above 115/75 mmHg and increases progressively. The reason 130/80 mmHg is set as the diagnostic threshold for Stage 1 hypertension isn’t that risk suddenly appears there – it’s that above this level, the evidence for benefit from treatment becomes robust enough to justify intervention.
Can complications be reversed once they’ve started? Some changes are partially reversible with treatment – LVH can regress, proteinuria can decrease, and atherosclerosis progression can be slowed. But established scarring (fibrosis in the heart, kidneys, or brain), significant atherosclerotic plaque, and completed strokes represent permanent damage. This is the core argument for treating hypertension early, before structural changes become entrenched.
Do blood pressure medications prevent complications even if they have side effects? For most people, yes – the cardiovascular and kidney protection from effective blood pressure lowering outweighs the side effect profile of most antihypertensive medications, which are generally well tolerated. If a specific medication causes problematic side effects, there are many alternatives – the key is finding an effective regimen, not tolerating one that’s bothersome. Discuss this directly with your doctor rather than stopping medication on your own.
Is stroke from hypertension preventable? Largely yes. The majority of strokes are considered preventable with adequate blood pressure control, anticoagulation for AFib where appropriate, and management of other stroke risk factors. The potential for prevention is precisely why population-level blood pressure control is considered one of the highest-value interventions in cardiovascular medicine.
Does hypertension cause vision loss? Advanced hypertensive retinopathy can cause visual disturbances and in severe cases vision loss. However, most hypertensive retinopathy doesn’t reach this stage if blood pressure is reasonably controlled. Routine fundoscopic examination (looking at the back of the eye) can detect early retinal changes in asymptomatic patients, which is one reason regular eye exams have value beyond vision correction.
Disclaimer
This article is for educational purposes only and does not constitute medical advice. Hypertension management and cardiovascular risk reduction should be directed by a qualified healthcare provider. Do not adjust medications or make health decisions based solely on this content without medical guidance.
References
- Whelton PK, et al. 2017 ACC/AHA high blood pressure guideline. Journal of the American College of Cardiology. 2018;71(19):e127-e248. https://doi.org/10.1016/j.jacc.2017.11.006
- Feigin VL, et al. Global and regional burden of stroke during 1990-2010: findings from the Global Burden of Disease Study 2010. The Lancet. 2014;383(9913):245-254. https://doi.org/10.1016/S0140-6736(13)61953-4
- Lewington S, et al. Age-specific relevance of usual blood pressure to vascular mortality. The Lancet. 2002;360(9349):1903-1913. https://doi.org/10.1016/S0140-6736(02)11911-8
- SPRINT MIND Investigators. Effect of intensive vs standard blood pressure control on probable dementia. JAMA. 2019;321(6):553-561. https://doi.org/10.1001/jama.2018.21442
- Thomopoulos C, Parati G, Zanchetti A. Effects of blood pressure-lowering on outcome incidence in hypertension. Journal of Hypertension. 2014;32(12):2285-2295. https://doi.org/10.1097/HJH.0000000000000378
- American Heart Association. Consequences of high blood pressure. https://www.heart.org/en/health-topics/high-blood-pressure/health-threats-from-high-blood-pressure
- Centers for Disease Control and Prevention (CDC). High blood pressure and related conditions. https://www.cdc.gov/bloodpressure/health_problems.htm
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). High blood pressure and kidney disease. https://www.niddk.nih.gov/health-information/kidney-disease/high-blood-pressure
- Messerli FH, Rimoldi SF, Bangalore S. The transition from hypertension to heart failure. JACC: Heart Failure. 2017;5(8):543-551. https://doi.org/10.1016/j.jchf.2017.04.012
- National Institutes of Health (NIH). Cognitive health and high blood pressure. https://www.nia.nih.gov/health/high-blood-pressure-and-older-adults