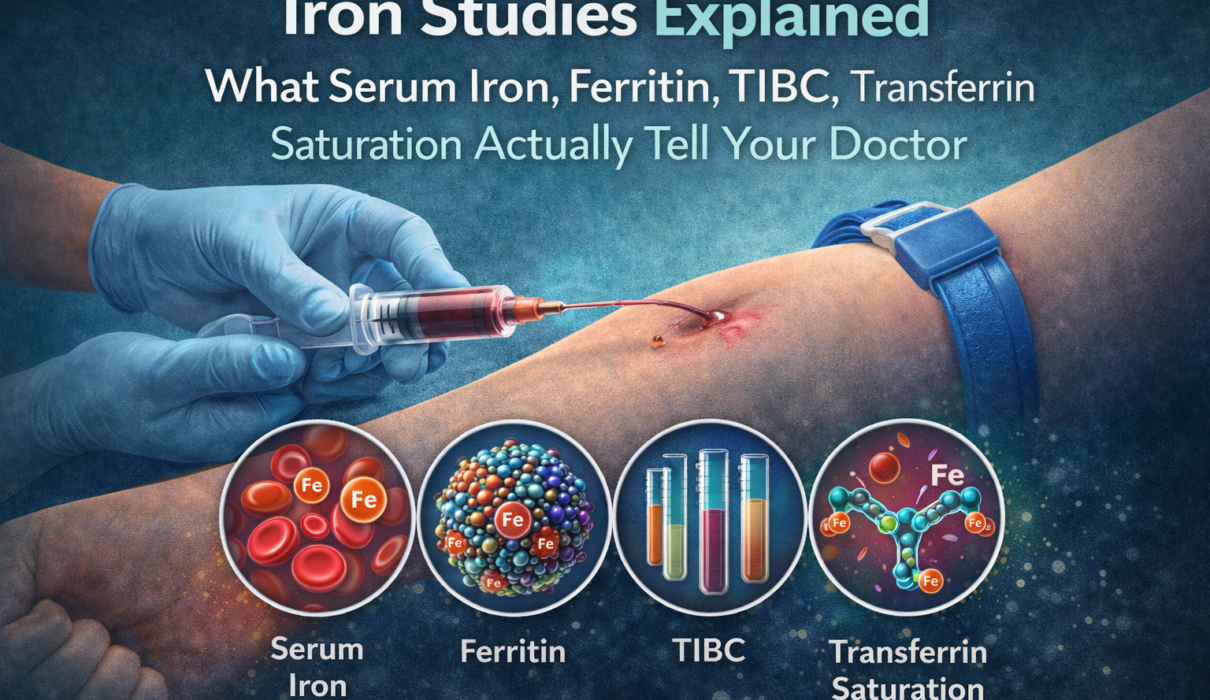
You get a blood test. The report comes back with four or five numbers – serum iron, ferritin, TIBC, transferrin saturation – and none of them seem to be telling the same story. One is low. Another is high. Your doctor says something about iron deficiency, but you’re not sure what any of these markers actually measure or why you need all of them.
That confusion is completely reasonable. Iron metabolism is genuinely a multi-step process, and each marker in an iron panel is looking at a different part of it. Serum iron alone doesn’t give you the full picture. Neither does ferritin alone. You need the whole panel – and you need to understand what each piece is measuring – to make sense of what’s happening.
This article breaks down exactly that: what each marker measures, what the numbers mean, what patterns to look for, and when iron studies are ordered in the first place.
Why Iron Needs Multiple Tests
Iron doesn’t just float freely in your blood. It moves through a carefully regulated system involving carrier proteins, storage proteins, and constant feedback between your gut, bone marrow, and liver. To understand where that system is breaking down, you need to look at more than one point.
Here’s the basic chain: Iron from food is absorbed in your small intestine, picked up by a transport protein called transferrin, and carried through the bloodstream to wherever it’s needed – primarily the bone marrow, where it’s used to make hemoglobin in new red blood cells. Iron that isn’t immediately used gets packaged into a storage protein called ferritin, mostly in the liver, spleen, and muscle tissue. The body draws on those stores when supply is tight.
Each marker in the iron panel reflects a different step in this chain:
- Serum iron measures the amount of iron currently circulating in your blood, bound to transferrin
- Transferrin (or its proxy, TIBC) measures how much transport capacity your blood has
- Transferrin saturation tells you how much of that transport capacity is currently being used
- Ferritin tells you how much iron is sitting in storage
No single number tells the whole story. A normal serum iron with a critically low ferritin means your circulating iron looks fine today, but your reserves are nearly empty. A high ferritin with a low serum iron might mean iron deficiency – or it might mean inflammation. You have to read them together.
Serum Iron
Serum iron measures the amount of iron circulating in your blood plasma at the time of the blood draw – specifically, the iron that’s bound to transferrin and available for use.
Normal range: approximately 60-170 mcg/dL for adults (ranges vary slightly by lab and sex)
What affects it: Serum iron fluctuates a lot, and that’s one of its main limitations as a standalone marker. It varies throughout the day – levels are typically higher in the morning and lower in the evening. A single high-iron meal can raise it temporarily. Illness, inflammation, and recent blood transfusions all affect it. This is why iron studies are ideally drawn fasting, in the morning, and interpreted alongside the other markers rather than in isolation.
When it’s low: Low serum iron suggests the body isn’t getting enough iron into circulation. This happens in iron deficiency, but also in chronic inflammatory conditions (where iron gets trapped in storage and isn’t released normally – more on that below).
When it’s high: Elevated serum iron can indicate iron overload disorders like hereditary hemochromatosis, liver disease, or – in acute cases – iron poisoning.
The key limitation: Serum iron is the least reliable marker on its own. A single reading can look normal even in moderate iron deficiency, and can look abnormal for reasons that have nothing to do with iron status. Always interpret it with ferritin and TIBC.
Ferritin
Ferritin is the protein that stores iron inside cells. The ferritin level in your blood reflects how much iron is sitting in those storage reserves – primarily in the liver, bone marrow, and spleen.
Normal range: approximately 12-300 ng/mL for men; 12-150 ng/mL for women (lab reference ranges vary)
Ferritin is the single most sensitive early marker for iron deficiency. Long before serum iron drops and long before hemoglobin falls enough to produce anemia, ferritin starts declining as the body draws on its stores to compensate for inadequate intake. A ferritin below 12 ng/mL is strongly diagnostic of iron deficiency. Many clinicians and guidelines, including recommendations from the American Society of Hematology, now use a threshold of 30 ng/mL as the lower limit of optimal iron stores, particularly in women and people with ongoing losses.
When it’s low: Depleted iron stores – from insufficient dietary intake, blood loss (menstruation, gastrointestinal bleeding, frequent blood donation), malabsorption (celiac disease, post-bariatric surgery), or increased demand (pregnancy, growth).
When it’s high: This is where ferritin becomes complicated. Because ferritin is also an acute-phase reactant – a protein that rises during inflammation, infection, and tissue injury – elevated ferritin doesn’t always mean iron overload. High ferritin can reflect:
- Hereditary hemochromatosis (genetic iron overload disorder)
- Chronic liver disease
- Active inflammation, infection, or autoimmune conditions
- Certain cancers
- Metabolic syndrome and type 2 diabetes
- Adult-onset Still’s disease (a rare inflammatory condition where ferritin can reach extremely high levels)
This is why a high ferritin needs context. Someone with ferritin of 400 ng/mL and active rheumatoid arthritis is in a very different situation than someone with the same ferritin and no inflammatory disease.
TIBC – Total Iron-Binding Capacity
TIBC measures how much iron your blood could potentially carry – in other words, it’s a measure of total transport capacity. Because transferrin is the main protein that carries iron in the blood, TIBC is essentially an indirect measure of transferrin levels. When transferrin is high, TIBC is high. When transferrin is low, TIBC is low.
Normal range: approximately 250-370 mcg/dL
The body upregulates transferrin production (and therefore increases TIBC) when iron stores are depleted – it’s trying to capture more iron from whatever is available. When iron is abundant, transferrin production falls and TIBC drops.
This inverse relationship is one of the most useful patterns in the iron panel:
- High TIBC = the body is hungry for iron, transferrin is ramping up to capture more = suggests iron deficiency
- Low TIBC = iron is plentiful (or the liver, which makes transferrin, isn’t functioning well) = suggests iron overload, chronic disease, or liver disease
Important caveat: TIBC can be low in chronic inflammatory conditions even when iron deficiency is present, because inflammation suppresses transferrin production. This is one reason why TIBC can be misleading in people with chronic illness – it won’t always rise the way you’d expect in iron deficiency.
Some labs report UIBC (unsaturated iron-binding capacity) instead of or alongside TIBC. UIBC measures the portion of transferrin that doesn’t currently have iron attached to it. TIBC = serum iron + UIBC.
Transferrin Saturation
Transferrin saturation is a calculated value – serum iron divided by TIBC, expressed as a percentage. It tells you what fraction of transferrin’s iron-carrying capacity is currently occupied.
Formula: Transferrin Saturation (%) = (Serum Iron ÷ TIBC) × 100
Normal range: approximately 20-50%
Under normal conditions, about one-third of transferrin’s binding sites are occupied with iron, with the rest held in reserve. When iron is scarce, saturation falls. When iron is excessive, saturation rises.
When it’s low (below 20%): Suggests insufficient iron supply relative to transport capacity – consistent with iron deficiency or, in the context of low TIBC and normal/high ferritin, anemia of chronic disease.
When it’s high (above 50%): Suggests iron overload or reduced transport capacity. A transferrin saturation consistently above 45% is one of the earliest markers flagged in hereditary hemochromatosis screening – often rising before ferritin becomes significantly elevated.
Transferrin saturation is particularly useful in two situations: screening for hemochromatosis (high saturation is the key early finding) and differentiating iron deficiency anemia from anemia of chronic disease (more on that in the next section).
Reading the Panel Together: Common Patterns
This is where the real clinical value lies. Individual markers mean much less than the pattern across all four.
| Condition | Serum Iron | Ferritin | TIBC | Transferrin Sat. |
|---|---|---|---|---|
| Iron deficiency (early) | Normal | Low | High | Normal to low |
| Iron deficiency anemia | Low | Low | High | Low (<15%) |
| Anemia of chronic disease | Low | Normal/High | Low/Normal | Low/Normal |
| Hereditary hemochromatosis | High | High | Low | High (>45%) |
| Pregnancy | Low/Normal | Low/Normal | High | Low/Normal |
| Liver disease (acute hepatitis) | High | High | Variable | High |
| Chronic liver disease/cirrhosis | Variable | High | Low | Variable |
| Iron supplementation | High | Rising | Falling | High |
The tricky scenario – iron deficiency vs. anemia of chronic disease:
This distinction matters clinically because the treatments are different. In pure iron deficiency, ferritin is low and TIBC is high. In anemia of chronic disease (ACD), ferritin is normal or elevated (because inflammation drives it up regardless of actual stores) and TIBC is low or normal (because chronic illness suppresses transferrin production). When both conditions exist simultaneously – which happens, for example, in someone with inflammatory bowel disease and iron deficiency – the picture becomes more complex. Some clinicians use the soluble transferrin receptor (sTfR) test in this situation, as it rises in true iron deficiency but is unaffected by inflammation.
A useful rule of thumb: Low ferritin almost always means iron deficiency. High ferritin does not always mean iron is adequate – it may just mean inflammation is present.
Who Gets Iron Studies Ordered – and Why
Iron studies are typically ordered when:
- A complete blood count (CBC) shows low hemoglobin, low hematocrit, or small red blood cells (low MCV) – findings consistent with iron deficiency anemia
- Someone has symptoms suggesting iron deficiency: fatigue, weakness, cold intolerance, brittle nails, hair loss, restless legs, pica (craving non-food substances like ice)
- Someone is in a higher-risk group for iron deficiency: women with heavy menstrual periods, pregnant women, vegetarians/vegans, people with celiac disease or inflammatory bowel disease, frequent blood donors, long-distance runners
- A CBC or clinical picture suggests possible iron overload: joint pain, fatigue, elevated liver enzymes, family history of hemochromatosis
- Monitoring response to iron supplementation or treatment for hemochromatosis
- Evaluating unexplained fatigue where both deficiency and overload are possible
Before the test: Most labs recommend fasting for 8-12 hours before iron studies, ideally drawn in the morning. Iron supplements should typically be held for 24 hours beforehand (confirm with your ordering provider). Recent illness, inflammation, or blood transfusion can affect results and should be flagged when interpreting them.
Reference Ranges: What the Numbers Look Like
Reference ranges vary between laboratories, so always interpret your results against the ranges printed on your own lab report. These are approximate adult ranges used as general reference:
| Test | Approximate Normal Range | Notes |
|---|---|---|
| Serum Iron | 60-170 mcg/dL | Lower in women; varies by time of day |
| Ferritin | 12-300 ng/mL (men); 12-150 ng/mL (women) | Highly variable by sex and age |
| TIBC | 250-370 mcg/dL | Rises in deficiency; falls in overload/chronic disease |
| Transferrin Saturation | 20-50% | >45% warrants hemochromatosis evaluation |
Women, particularly those of reproductive age, tend to have lower ferritin and serum iron reference ranges than men. Many clinicians argue that conventional lower limits for ferritin (like 12 ng/mL) are set too low for women, and that symptoms of iron insufficiency can occur at ferritin levels between 12-30 ng/mL – a range some labs would still call “normal.”
Frequently Asked Questions
Can ferritin be normal but I still be iron deficient? Yes. Ferritin is an acute-phase reactant, meaning it rises with inflammation, infection, or chronic illness. If you have an underlying inflammatory condition, ferritin can read as normal or even elevated even when your actual iron stores are low. In this scenario, transferrin saturation and soluble transferrin receptor (sTfR) can provide more accurate information about true iron stores.
Why is my serum iron normal but my ferritin is low? This is actually a common early-stage finding. When iron stores first start to deplete, the body compensates by pulling iron from ferritin reserves and increasing transferrin production to capture more from circulation. Serum iron can stay in the normal range while ferritin falls – which is why ferritin is a more sensitive early marker for iron deficiency than serum iron.
What does a high ferritin with normal iron studies mean? Isolated elevated ferritin – particularly when serum iron and transferrin saturation are normal – most commonly reflects inflammation rather than true iron overload. Common causes include obesity, metabolic syndrome, fatty liver disease, alcohol use, and any acute or chronic inflammatory condition. It warrants investigation if it’s significantly elevated, but doesn’t automatically mean hemochromatosis.
How quickly do iron studies improve after starting supplements? Serum iron and transferrin saturation typically improve within days to a few weeks of starting iron supplementation. Ferritin takes longer – it can take 3-6 months of consistent supplementation to meaningfully rebuild iron stores, depending on how depleted they were. Hemoglobin, if it was low, typically starts to rise within 2-4 weeks but may take 2-3 months to fully normalize.
Should I be concerned about a high transferrin saturation? A consistently elevated transferrin saturation – particularly above 45% – warrants follow-up, as it’s one of the earliest findings in hereditary hemochromatosis. If found, your doctor will typically check ferritin, repeat the test on a different occasion, and may order genetic testing for the HFE gene mutations associated with hemochromatosis. A single elevated reading isn’t diagnostic on its own.
Disclaimer
This article is intended for general informational and educational purposes only and does not constitute medical advice. Iron studies results must be interpreted by a qualified healthcare provider in the context of your full clinical picture, symptoms, and medical history. Do not adjust iron supplementation or stop any treatment based on this content without consulting your doctor.
References
- Camaschella C. Iron-deficiency anemia. New England Journal of Medicine. 2015;372(19):1832-1843. https://doi.org/10.1056/NEJMra1401038
- Peng YY, Uprichard J. Ferritin and iron studies in anaemia and chronic disease. Journal of Clinical Pathology. 2017;70(1):6-11. https://doi.org/10.1136/jclinpath-2016-203805
- U.S. National Library of Medicine – MedlinePlus. Iron Tests. https://medlineplus.gov/lab-tests/iron-tests/
- Labcorp. Iron and Total Iron-binding Capacity (TIBC). https://www.labcorp.com/tests/001321/iron-and-total-iron-binding-capacity-tibc
- Cleveland Clinic. Total Iron-Binding Capacity (TIBC). https://my.clevelandclinic.org/health/diagnostics/24979-total-iron-binding-capacity-tibc
- Pasricha SR, Tye-Din J, Muckenthaler MU, Swinkels DW. Iron deficiency. The Lancet. 2021;397(10270):233-248. https://doi.org/10.1016/S0140-6736(20)32594-0
- Ganz T. Anemia of inflammation. New England Journal of Medicine. 2019;381(12):1148-1157. https://doi.org/10.1056/NEJMra1903513
- Adams PC, Barton JC. Haemochromatosis. The Lancet. 2007;370(9602):1855-1860. https://doi.org/10.1016/S0140-6736(07)61782-6
- National Heart, Lung, and Blood Institute. Iron-Deficiency Anemia. https://www.nhlbi.nih.gov/health/anemia/iron-deficiency-anemia
- American Society of Hematology. Iron-Deficiency Anemia. https://www.hematology.org/education/patients/anemia/iron-deficiency