If you have PCOS, there is a very good chance that insulin resistance is part of your picture – even if nobody has mentioned it to you.
It doesn’t show up dramatically. You don’t necessarily feel it happening. Your blood sugar might look completely normal on a standard test. But underneath that normal-looking number, something significant may be going on in the way your body handles glucose and regulates hormones – and understanding it changes how PCOS makes sense and what you can do about it.
Insulin resistance is present in an estimated 65 to 70 percent of women with PCOS – making it one of the most consistent and most important features of the condition (Diamanti-Kandarakis and Dunaif, 2012). It is also one of the least explained. Many women with PCOS are told they have the condition, given a prescription for the pill or metformin, and sent home without anyone clearly explaining what insulin resistance actually is, why it matters beyond blood sugar, and why it’s connected to what seems like a completely different problem – irregular periods and hormonal imbalance.
This article explains that connection clearly.
This article is part of our PCOS series. For the full overview of the condition, visit our PCOS Explained guide.
What Insulin Actually Does
Before getting into insulin resistance, it helps to understand what insulin is supposed to do – because the failure of the system makes a lot more sense once you understand what the system is trying to accomplish.
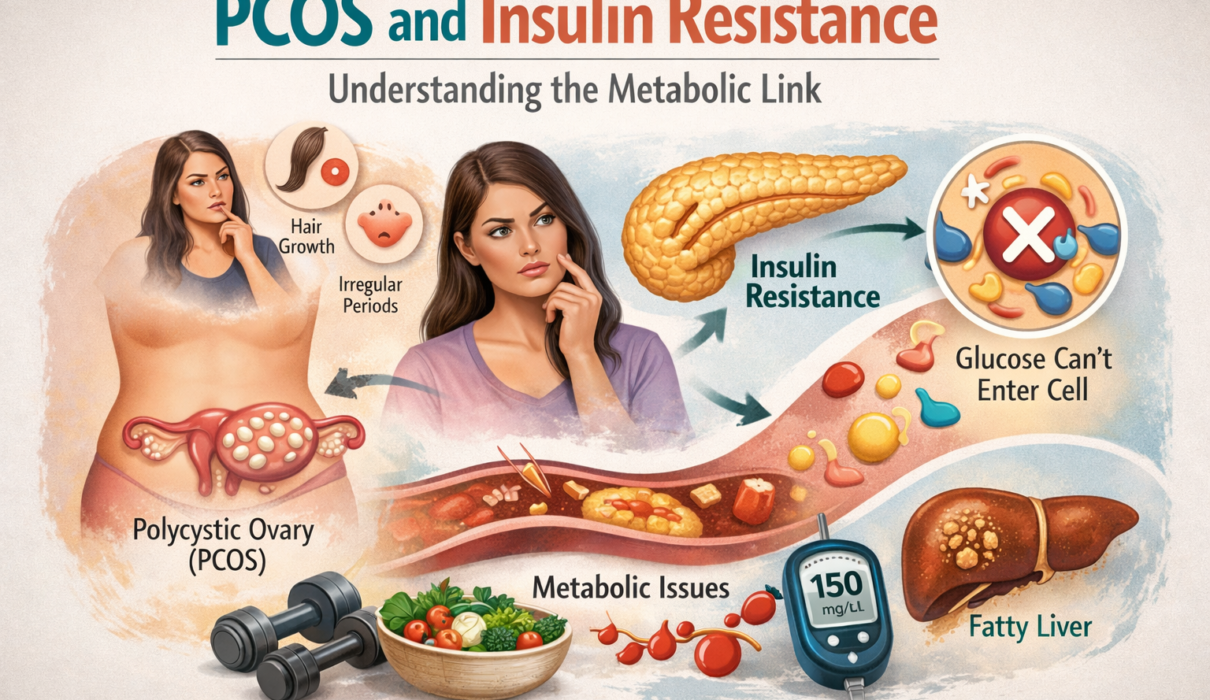
Insulin is a hormone produced by the pancreas in response to rising blood sugar. After you eat – particularly after eating carbohydrates – glucose enters the bloodstream. Insulin acts as a key, unlocking the doors of cells throughout the body to allow glucose to enter and be used for energy. Without insulin doing its job, glucose can’t get into cells and builds up in the bloodstream instead.
In a healthy system, this process is efficient and self-regulating. You eat, blood sugar rises, insulin is released, glucose enters cells, blood sugar returns to normal, insulin levels drop back down.
Insulin resistance disrupts this system at the cellular level. The cells – particularly in muscle, liver, and fat tissue – become less responsive to insulin’s signal. The key still works, but the locks have become stiff and don’t open as easily. The pancreas compensates by producing more insulin – essentially sending more keys to try to open the same stubborn locks. Blood sugar may stay in the normal range because the pancreas is working hard enough to compensate. But insulin levels are chronically elevated. And that chronic elevation has consequences that extend far beyond blood sugar.
“Insulin resistance doesn’t always show up on a standard blood sugar test – because the pancreas compensates by producing more insulin. But that elevated insulin has consequences throughout the body that go well beyond glucose regulation.”
The Link Between Insulin Resistance and PCOS: How They Drive Each Other
This is the part that most PCOS conversations skip over – and it’s the most important part of the metabolic picture.
Chronically elevated insulin levels have a specific and significant effect on the ovaries: they stimulate the ovarian theca cells to produce more androgens – male sex hormones, primarily testosterone. This happens through two mechanisms. First, elevated insulin directly signals the ovaries to ramp up androgen production. Second, elevated insulin reduces levels of sex hormone-binding globulin (SHBG) – a protein that normally binds testosterone in the bloodstream and keeps it inactive. Less SHBG means more free, biologically active testosterone circulating in the body.
The result is elevated androgen levels – which disrupt the normal follicle development process in the ovaries, prevent ovulation from occurring reliably, and cause the hormonal imbalance that produces PCOS symptoms.
And here is where the cycle closes: elevated androgens themselves worsen insulin resistance, creating a reinforcing loop where each side makes the other worse.
| Insulin resistance causes | Which leads to |
|---|---|
| Elevated insulin levels | Ovarian androgen overproduction |
| Reduced SHBG | Higher free testosterone levels |
| Higher androgen levels | Further disruption of ovulation |
| Anovulation | Irregular periods, follicle accumulation |
| More androgen excess | Worsened insulin resistance |
This cycle explains something that confuses many women with PCOS: why treating the insulin resistance – through metformin, lifestyle changes, or inositol supplementation – often improves menstrual regularity and hormonal balance, even though those seem like reproductive problems rather than metabolic ones. The hormonal and metabolic systems in PCOS are not separate problems. They are the same problem expressing itself through different pathways.
The Lean PCOS Problem: Insulin Resistance Without Obesity
One of the most important and most misunderstood facts about insulin resistance in PCOS is that it is not caused by or limited to excess weight.
Approximately 20 to 30 percent of women with PCOS are lean – and lean women with PCOS have insulin resistance at rates comparable to overweight women with the condition (Yildiz et al., 2012). The insulin resistance in PCOS appears to be driven primarily by intrinsic cellular signaling abnormalities – something happening at the level of how cells respond to insulin – rather than simply by excess fat tissue.
This matters enormously because it means:
- Lean women with PCOS can have significant metabolic risk that goes unrecognized because providers associate insulin resistance with obesity
- Weight is not the primary driver of insulin resistance in PCOS – and losing weight is not the only way to address it
- Metabolic monitoring is appropriate for all women with PCOS, regardless of body size
- The recommendation to “just lose weight” as the solution to PCOS is both incomplete and sometimes entirely beside the point
“Insulin resistance in PCOS is not caused by being overweight. Lean women with PCOS have it too – driven by cellular signaling abnormalities that exist independently of body weight. This is why metabolic assessment matters for every woman with PCOS, not just those who are overweight.”
What Insulin Resistance Feels Like – and What It Doesn’t
Insulin resistance in PCOS is typically silent in its early stages. There are no dramatic symptoms that announce its presence. But over time – and sometimes earlier than people expect – certain signs can emerge.
Signs that may suggest insulin resistance in PCOS:
- Fatigue after meals – particularly after high-carbohydrate meals; a crash in energy an hour or two after eating is a common experience
- Cravings for sugar and carbohydrates – insulin resistance disrupts the normal feedback between blood sugar and appetite, often producing persistent cravings
- Difficulty losing weight – particularly around the abdomen, despite diet and exercise changes
- Acanthosis nigricans – darkening and thickening of the skin in body folds like the neck, armpits, or groin; a visible sign of elevated insulin levels
- Brain fog – difficulty concentrating, particularly in the afternoon
- Irregular periods – a consequence of the androgen-ovulation disruption described above
- Acne and excess hair growth – driven by the elevated androgens that insulin resistance promotes
None of these symptoms are definitive on their own. And as noted, many women with insulin resistance in PCOS have none of these symptoms at all. But recognizing the pattern helps prompt the right investigation.
How Insulin Resistance Is Assessed
Assessing insulin resistance is not as straightforward as checking a standard blood sugar level – which is part of why it is so frequently missed.
A normal fasting blood glucose does not rule out insulin resistance. Because the pancreas compensates by producing more insulin, blood sugar can remain in the normal range for years while insulin resistance is significant and worsening. By the time fasting glucose becomes abnormal, the pancreas has often been overworking for a long time.
Tests used to assess insulin resistance and metabolic risk in PCOS:
| Test | What it measures | What it tells you |
|---|---|---|
| Fasting glucose | Blood sugar after an overnight fast | Screens for prediabetes; can be normal with significant insulin resistance |
| Fasting insulin | Insulin level after an overnight fast | Elevated fasting insulin suggests insulin resistance even with normal glucose |
| HbA1c | Average blood sugar over 3 months | Identifies prediabetes and diabetes; more stable than single glucose reading |
| Oral glucose tolerance test (OGTT) | Blood sugar and insulin response to a glucose drink | Most sensitive test for detecting early insulin resistance and glucose dysregulation |
| HOMA-IR | Calculated index using fasting glucose and insulin | Quantifies degree of insulin resistance; useful for tracking change over time |
| Lipid panel | Cholesterol and triglycerides | Insulin resistance typically causes elevated triglycerides and low HDL |
The oral glucose tolerance test – which involves drinking a glucose solution and measuring blood sugar and insulin at intervals over two hours – is significantly more sensitive than fasting glucose alone for detecting insulin resistance and glucose dysregulation in PCOS. If your evaluation has only included a standard fasting glucose or HbA1c, asking specifically about an OGTT is entirely reasonable.
The Long-Term Health Implications
Understanding insulin resistance in PCOS matters not just for managing current symptoms but for long-term health. Chronically elevated insulin and the metabolic disruption it causes significantly increase the risk of several serious conditions over time.
Women with PCOS face:
- 4 to 8 times the risk of type 2 diabetes compared to women without PCOS – one of the most significant metabolic risks associated with the condition
- Higher rates of prediabetes – often detectable years before diabetes develops
- Dyslipidemia – elevated triglycerides and reduced HDL cholesterol, the pattern most associated with insulin resistance
- Higher rates of hypertension and cardiovascular disease risk factors
- Non-alcoholic fatty liver disease (NAFLD) – increasingly recognized as a consequence of insulin resistance in PCOS
- Metabolic syndrome – the cluster of metabolic risk factors that significantly increases cardiovascular risk
These are long-term risks that unfold over decades – not immediate consequences. But they are worth taking seriously because they are largely preventable or modifiable with early attention. A woman with PCOS who is aware of her metabolic risk and manages it appropriately has a dramatically different long-term trajectory than one who never had the conversation.
What Actually Helps: Addressing Insulin Resistance in PCOS
The good news is that insulin resistance in PCOS is genuinely responsive to intervention – both lifestyle-based and medical. And because the metabolic and hormonal systems are connected, improving insulin sensitivity often improves hormonal balance, menstrual regularity, and PCOS symptoms at the same time.
Lifestyle Approaches
Exercise is one of the most powerful tools for improving insulin sensitivity – and it doesn’t require dramatic amounts to make a difference. Both aerobic exercise and resistance training improve insulin sensitivity through different mechanisms, and combining both produces the greatest benefit. Even moderate amounts – 150 minutes of moderate-intensity activity per week as recommended by the American Heart Association – produce measurable improvements in insulin sensitivity.
Diet significantly influences insulin levels and insulin sensitivity. The key principles for women with PCOS are:
- Prioritizing lower glycemic index carbohydrates that produce a more gradual rise in blood sugar and insulin
- Eating protein at each meal – protein reduces post-meal glucose spikes and improves satiety
- Including healthy fats – which slow glucose absorption and support satiety
- Limiting ultra-processed foods, sugary drinks, and refined carbohydrates that produce rapid insulin spikes
- The Mediterranean dietary pattern has the strongest evidence base for PCOS specifically (Barrea et al., 2021)
Sleep has a direct effect on insulin sensitivity that is frequently overlooked. Even short-term sleep deprivation impairs insulin signaling. Women with PCOS already have higher rates of sleep disorders including sleep apnea – addressing sleep quality is a meaningful metabolic intervention, not just a lifestyle preference.
Stress management matters because chronic cortisol elevation from sustained stress impairs insulin sensitivity and promotes central fat storage. This is not a trivial contributor for many women with PCOS.
Medical Approaches
Metformin is the most widely used medication for addressing insulin resistance in PCOS in the United States. It is an insulin sensitizer that reduces the amount of glucose the liver produces and improves cellular insulin sensitivity. In PCOS, metformin improves insulin resistance, reduces androgen levels, can help restore ovulation, and lowers long-term metabolic risk. It is not a diabetes medication exclusively – it is used throughout PCOS management even in women with normal blood sugar levels.
Inositol – specifically the combination of myo-inositol and D-chiro-inositol – is a supplement with a meaningful and growing evidence base for improving insulin sensitivity in PCOS. Multiple randomized trials have shown benefits including reduced fasting insulin, improved hormonal parameters, and restored ovulation in some women (Unfer et al., 2017). It is not FDA-approved specifically for PCOS but is widely used and has a favorable safety profile.
GLP-1 receptor agonists – medications including semaglutide (Ozempic, Wegovy) and liraglutide (Victoza, Saxenda) – are attracting significant research interest in PCOS given their effects on insulin sensitivity, weight, and potentially androgen levels. Evidence in PCOS specifically is growing but not yet sufficient to make them standard treatment. Their use in PCOS is currently off-label and should be discussed with an endocrinologist or specialist.
Frequently Asked Questions
Q: My blood sugar is completely normal. Does that mean I don’t have insulin resistance?
Not necessarily. Normal fasting blood glucose is compatible with significant insulin resistance – particularly early in its course, when the pancreas is still compensating effectively. A fasting insulin level, HOMA-IR calculation, or oral glucose tolerance test is more sensitive for detecting insulin resistance before blood sugar becomes abnormal. If you have PCOS and haven’t had these tests, asking your provider specifically about insulin resistance assessment is worthwhile.
Q: I’m not overweight. Should I still be concerned about insulin resistance?
Yes. Insulin resistance in PCOS is present in lean women at rates similar to overweight women – it is driven by cellular signaling abnormalities rather than body fat alone. Lean women with PCOS have the same long-term metabolic risks and benefit from the same metabolic monitoring and interventions as overweight women with the condition.
Q: Will taking metformin make me lose weight?
Metformin can support modest weight loss in some people, primarily through its effects on appetite and glucose metabolism. It is not a weight loss medication in the primary sense, and its weight effects in PCOS are modest and variable. Its primary value in PCOS is improving insulin sensitivity, reducing androgen levels, and lowering long-term metabolic risk – not weight loss specifically.
Q: Can inositol replace metformin for insulin resistance in PCOS?
For some women with milder insulin resistance, inositol supplementation – particularly myo-inositol combined with D-chiro-inositol – produces meaningful improvements in insulin sensitivity and hormonal parameters. For women with more significant insulin resistance or metabolic risk, metformin has a stronger evidence base. Many providers use them in combination. This is a conversation worth having with your provider based on your specific labs and clinical picture.
Q: If I address my insulin resistance, will my periods become regular?
For many women with PCOS, yes – improving insulin sensitivity through lifestyle changes, metformin, or inositol can restore more regular ovulation and menstrual cycles, because the androgen excess driving the disruption is partly fueled by elevated insulin. The effect is not universal and depends on the severity of the underlying hormonal disruption, but improved insulin sensitivity is one of the most reliable pathways to improved menstrual regularity in PCOS.
Disclaimer: This article is for educational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for personal health concerns.
References
Diamanti-Kandarakis E, Dunaif A. Insulin resistance and the polycystic ovary syndrome revisited: an update on mechanisms and implications. Endocr Rev. 2012;33(6):981-1030. https://pubmed.ncbi.nlm.nih.gov/23065822
Yildiz BO, Bozdag G, Yapici Z, Esinler I, Yarali H. Prevalence, phenotype and cardiometabolic risk of polycystic ovary syndrome under different diagnostic criteria. Hum Reprod. 2012;27(10):3067-3073. https://pubmed.ncbi.nlm.nih.gov/22777527
Barrea L, Marzullo P, Muscogiuri G, et al. Source and amount of carbohydrate in the diet and inflammation in women with polycystic ovary syndrome. Nutr Res Rev. 2021;34(1):1-12. https://pubmed.ncbi.nlm.nih.gov/31937382
Unfer V, Carlomagno G, Dante G, Facchinetti F. Effects of myo-inositol in women with PCOS: a systematic review of randomized controlled trials. Gynecol Endocrinol. 2012;28(7):509-515. https://pubmed.ncbi.nlm.nih.gov/22296306
Teede HJ, Misso ML, Costello MF, et al. Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Hum Reprod. 2018;33(9):1602-1618. https://pubmed.ncbi.nlm.nih.gov/30052961
Endocrine Society. Polycystic Ovary Syndrome Clinical Practice Guideline. 2023. https://www.endocrine.org/clinical-practice-guidelines/polycystic-ovary-syndrome
American Diabetes Association. Standards of Medical Care in Diabetes. 2023. https://diabetesjournals.org/care/issue/46/Supplement_1





7 Comments